Covid-19 Length of Hospital Stay a Systematic Review and Data Synthesis
- Research
- Open Admission
- Published:
Factors associated with length of stay in intendance homes: a systematic review of international literature
Systematic Reviews volume 8, Article number:56 (2019) Cite this article
Abstruse
Background
A number of studies have explored factors associated with resident length of stay in care homes; however the findings of these studies take not been synthesized. The aim of this paper is to provide a systematic review of factors associated with length of stay until death and the strength of testify supporting each of these factors.
Methodology
This is a systematic review; databases included MEDLINE, EMBASE, PsycINFO, CINAHL, Proquest, the Cochrane Library and Web of Scientific discipline were searched. Observational studies, either prospective or retrospective, that explored multiple factors associated with length of stay until death in care homes were included. Studies that met the inclusion criteria were sourced, data extracted and assessed for quality. Data synthesis combined the direction and significance of association with the quality of the written report, resulting in strong, moderate, weak or inconclusive evidence for each gene identified.
Results
Forty-seven studies were identified as coming together the inclusion criteria. After quality assessment, 14 studies were judged to exist of a high quality, 31 of a moderate quality and 2 of a low quality. Three factors had strong bear witness to support their clan with shorter lengths of stay: shortness of jiff, receipt of oxygen therapy and admission to a facility providing nursing care.
Conclusions
This review summarized the factors associated with length of stay. It found stronger evidence for physical performance existence associated with shorter lengths of stay than for cognitive functioning. An understanding of expected length of stay for older adults admitted to a care abode is important for estimating lifetime costs and the implications of reforming funding arrangements for social care. Further research is needed to explore heterogeneity in this area.
Groundwork
The global population is ageing; 35% of the European population and 28% of the Due north American population are expected to be anile 60 years or over by 2050 [i]. By 2030, the number of older persons in the globe is estimated to increase to 1.4 billion, resulting in ii.1 billion in 2050 and potentially 3.1 billion in 2100 [2]. Every bit a consequence of this growth, deaths in this population group volition also increment; among those fourscore years and older, deaths are projected to rise to over 15 one thousand thousand by 2030 [iii]. Providing intendance for an ageing, and dying, population is, and volition continue to be, a novel challenge for healthcare systems around the globe.
Older adults are more likely to be frail, have multiple comorbidities and suffer from chronic diseases, including dementia, than younger adults. Equally end of life approaches, common preference amidst older adults is to remain in the home until death [4]; however, this may not be possible for those requiring loftier levels of care or without access to formal or informal care providers. The bulk of deaths in older adults with dementia occur in long-term care facilities [5, 6]; in England and Wales, it is estimated that by 2040, care homes will go the most common place of decease [7]. Although terminology and typology vary between countries, a intendance home or long-term intendance facility generally refers to a collective institutional setting where care is provided to older adults, who alive in that location, 24 hours a day, vii days a week [eight]. The provision of care homes, in terms of type (with or without nursing), number of beds and staffing levels, provision of funding and human relationship with the wider health care organisation, besides varies between countries [8]. This newspaper will utilise the term care home throughout.
Transitions from living in the community to a care dwelling can exist varied, and reflective of individual circumstances, such equally health status, access to care and fiscal circumstances. A systematic review by Luppa et al. identified characteristics associated with admission into care homes from 36 prospective observational studies of population samples, which followed older adults in the customs to care domicile access [ix]. Older adults who enter care homes are more likely to be older, have lower self-rated health, functional impairments, cognitive impairments and dementia [9]. In some cases, admission may follow a long period of physical or cognitive decline leaving caregivers unable to provide the level of intendance required by the resident. In other cases, a trigger event, such as a stroke or autumn, may lead to a resident being unable to return to living independently in their ain dwelling.
Compared to older adults residing in the community, care habitation residents have poorer health, including higher rates of dementia, stroke and severe mental illness [10]. An increased utilise of health services is common; care home residents also accept high rates of hospital and emergency section access, primary care contact and use of out of hours services [11,12,thirteen]. In 2014, Barclay et al. conducted a prospective study following residents in six residential care homes until death and identified four trajectories towards end of life: anticipated dying, uncertain dying, unexpected decease and unpredicted dying [14]. Briefly, the trajectories were based on whether the resident's death was expected and the presence of a sudden illness or an acute event.
Despite these high healthcare needs, the availability of information on care homes and their residents varies internationally. Some countries have minimum datasets, such equally Minimum Data Fix in the U.s. [fifteen], which provide a wealth of routinely collected data for potential research. Data on intendance habitation residents may too be available in larger cohort studies, such as the English language Longitudinal Study of Ageing (ELSA) [xvi] or the Survey of Health, Ageing and Retirement in Europe (SHARE) [17]. All the same, care habitation residents are frequently excluded from datasets focusing on older adults; in the UK few observational studies either include care home residents at baseline or follow upwardly community-home residents into care homes [18]. Methodological challenges of conducting research with older adults in care homes have been described elsewhere, including recruitment barriers, difficulties engaging with staff and adapting to competing demands on fourth dimension and resources [19].
Length of stay from admission until death is a simple measure that could inform our understanding of intendance domicile residents and identify variation in health service use. Length of stay is ofttimes reported as an event in care habitation research; notwithstanding, there is piffling consensus on the factors associated with length of stay, or how length of stay varies among residents, nationally and internationally. Building on the European Clan for Palliative Care Taskforce on Palliative Care in Long-term Care Settings for Older People [20], Froggatt et al. conducted a survey of palliative care provision in long-term care facilities in 29 European countries [21]. Data on average length of stay was returned by 14 countries (48%) and ranged from 63 days (Israel) to over 2000 days (Luxembourg). Using an average to report length of stay can be misleading; a minority of residents residing in care homes for an extended period, sometimes over 10 years, tin skew an average measure out, eclipsing residents admitted for very short periods of fourth dimension.
An understanding of length of stay data has several potential benefits: information technology can inform service planning to accommodate a growing number of residents and, combined with other measures, exist used to inform the provision of care within the wider health system. It can be used to identify variation across care homes, highlighting facilities with lengths of stay either below or above the expected based on the resident profile. Residents, their relatives and healthcare professionals could also do good from this information to inform controlling regarding relocation into long-term care, and equally a guide to support the provision and delivery of palliative care. Unlike mortality prediction tools, which accept been developed to help the identification of residents likely to die inside a specified time frame [22,23,24], an understanding of length of stay inside the care habitation population provides an overview of how care homes are being utilized by the older adults.
One previously conducted systematic review on length of stay in care home residents, conducted in 2013, identified five studies conducted in nursing homes; however, the review was limited to brusque-term bloodshed on health-related characteristics [25]. The aim of this newspaper is to systematically review the factors identified in observational studies as associated with length of stay in care homes.
Methodology
Identification of papers
A protocol for the systematic review was prepared prior to conducting the review. A systematic search strategy was developed and reported using criteria established in the Preferred Reporting Items for Systematic Review and Meta-Assay Protocols (PRISMA-P) 2015 argument [26]. The search strategy included a combination of gratuitous-text terms and subject indexing terms, such equally MeSH and EMTREE (Table 1). The search strategy was developed through identification of central terms in the titles and abstracts of relevant studies identified in an initial scoping search of the literature.
The following electronic databases were searched for manufactures published in peer-reviewed journals, from database inception to September 2016, and were not express by language or publication restrictions: MEDLINE, EMBASE, PsycINFO, Cumulative Index to Nursing and Allied Health Literature (CINAHL), Proquest, the Cochrane Library, including the Cochrane Methodology Register, Cochrane Central Annals of Controlled Trials (CENTRAL), Cochrane Database of Systematic Reviews (CDSR), Database of Abstracts of Reviews of Effect (DARE), Health Applied science Assessment (HTA) database and NHS Economic Evaluation Database (NHS EED), Web of Scientific discipline, the Campbell Library, SCOPUS and Social Intendance Online.
In cases where a conference abstract or unpublished research met the inclusion criteria, the lead writer was contacted where possible. Boosted papers were identified through other sources, including reviewing the reference lists of publications that met the inclusion criteria, reverse citation searches and gray literature. Reverse citation searches were undertaken on included papers using the ISI Spider web of Science Commendation Databases. Greyness literature was searched using OpenGrey. Websites were searched using an abbreviated search strategy; these included the World Health Arrangement, European Association of Palliative Intendance and Age Great britain.
Inclusion and exclusion criteria
The review focused on older adults, defined as any developed or groups of adults aged 65 years or above. Participants were included in the review if they resided in a care habitation or long-term care facility. As previously stated, the term "long-term intendance facility" more often than not refers to a collective institutional setting where care is provided to older people, who live there, 24 hours a twenty-four hour period, 7 days a week, equally defined previously [8]. In the review, this definition was likewise practical to care homes. Studies in hospitals, assisted living facilities, sheltered housing and hospices were excluded.
The review had one outcome measure, length of stay, divers as length of stay within a intendance abode until decease. Length of stay could exist measured in days, months, years or any other unit of time; and measured from whatever time point after admission. Studies exploring length of stay until belch were excluded. The review was restricted to observational studies, including retrospective or prospective cohort studies and case-control studies.
In the first stage of screening, a decision on whether a newspaper met the inclusion criteria was based on the study title and abstract. In the second stage of screening, a final decision on inclusion was fabricated based on reading the full paper.
In both stages, screening was conducted by one reviewer (DCM), and decisions checked by a blinded 2d reviewer (LD) on a subsample of x% of the papers. Discrepancies were discussed, and a last decision was made by a third member of the research squad (KF). Reasons for excluding full papers were recorded and reported (Fig. 1).
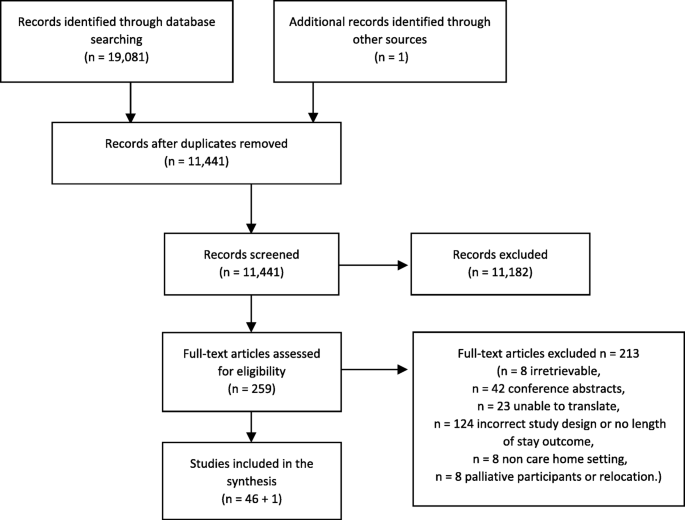
PRISMA flowchart
Data extraction
Information from the included studies were extracted using a data extraction class specifically developed for this review, informed past STROBE argument on the reporting of observational studies [27]. Data was extracted by one reviewer (DCM). The data nerveless from each report included: data on participants (number of residents, age of residents, gender of residents), the care home (type of care abode, number of intendance homes), the methodology (study setting, type of study, dataset used, information drove flow, follow up menstruation, how length of stay was divers, variables included in model, statistical method used) and information on missing data. The results of the newspaper, including take chances mensurate used and its value, confidence intervals and measure of significance were also extracted.
If a written report contained more than one cohort, both cohorts were included as dissever groups, such every bit Engle and Graney [28]. In evolution and validation studies, data from the development accomplice was extracted. In studies where men and women were listed separately, such as Hedinger, Hamming and Bopp, [29], the cohort that reflected the sample majority was used. In cases where the results were significant, either through significance testing or confidence intervals, the result was classed equally significant. In cases were no data on an included variable was reported in the results, the result was not pregnant or the confidence interval indicated none significance, the result was classed as non significant. If a study reported more than than one result for the same effect, i.e. historic period reported in groups, the result with either the well-nigh significant or the largest ratio was used to avert duplication. Factors included in less than three studies were excluded from the analysis to avoid bias in the evidence synthesis, which required a minimum of three studies to apply the information synthesis.
Quality assessment
There are numerous tools to appraise the methodological quality and take a chance of bias in randomized controlled trials; however, few are designed specifically for observational studies [30]. To ensure that the quality assessment tool was advisable for the topic area, the review used a modified version of the quality assessment tool used by Luppa et al., adapted for application to studies on factors associated with length of stay in intendance homes. The adapted tool has 14 items, scored as either 0 (not meeting the criteria) or 1 (meeting the criteria) (see Additional file 1). A score of 75% or more than of the assessment criteria was defined as high-quality studies, between fifty% and 75% was defined as moderate quality and less than l% was defined as low quality.
Data synthesis
Due to heterogeneity in the setting, sample and tools used, a meta-analysis was not advisable to synthesize the data. Information synthesis was split into ii stages. Firstly, the characteristics of the report were described, including the study design, sample size and variables reported. Numerical information was tabulated and presented for each factor, showing outcome size and direction.
Secondly, in a like approach used past Luppa et al., all factors identified across the studies were pooled and grouped, alongside the management of the variables effect on length of stay and their significance (positive, negative and not pregnant). These findings were and then cross-referenced with the quality assessment score for the study (encounter Additional files two and iii).
A judgment was made on the forcefulness of the testify for each risk factor from this cantankerous tabulation. A factor was classed as beingness supported by potent prove if there are consistent findings in at least 75% of studies in at least three high-quality studies. Moderate evidence was classed as consequent findings in at least 50% of studies in at least two high-quality studies. Weak bear witness was classed equally findings of one high-quality written report and of at to the lowest degree 2 moderate- to depression-quality studies or consistent findings (≥ 75%) in at least four or more moderate- to low-quality studies. If a take a chance factor was not classed every bit having strong, moderate or weak evidence, it was classed every bit inconclusive.
Results
The searches of the electronic databases identified 19,081 titles and abstracts, resulting in xi,441 afterwards deduplication. Based on applying the inclusion criteria to the abstract of the paper, 11,182 abstracts were excluded, identifying 259 abstracts for which full papers were sourced. Eight papers could non exist sourced, 42 were excluded as they were conference proceedings, 124 were excluded based on study blueprint or did not have a take a chance mensurate, 23 were in a language which could not exist translated by the research team, 8 were not conducted in care homes and 8 were exclusively in patients approaching end of life or concerned relocation. Ane newspaper was identified through other sources.
In total, 47 studies met the inclusion criteria for the review (Additional file 4). Study designs every bit reported past the papers included prospective studies (16), retrospective studies (thirteen), longitudinal, accomplice or follow-upward studies (8), secondary analysis, linked observational or population-based studies (iv) and case-control studies (2). Four papers did not report study design.
Seven of the 47 papers were split into more than 1 cohort, mostly through reporting follow-up for more i fourth dimension bespeak; each cohort was included in the synthesis separately resulting in 57 included cohorts from 47 papers. 1 year follow-up was based on 26 cohorts.
Xviii studies were conducted in the USA, x in Europe, 7 in the UK, 4 in Hong Kong, 2 in New Zealand and 5 elsewhere. Total sample size was 942,626, sample sizes ranged from 49 to 218,088, with 9 studies including residents with dementia, Alzheimer'south affliction or Parkinson's disease only. The majority of studies included residents anile over 65 years who were newly admitted to the facility. Average historic period ranged from 76.03 (x.08) to 92.ix (3.0), and the percent of the sample that was female ranged from 59.half dozen to 89.7%, where reported. In terms of how the report described the facility in which data were collected, 32 studies were based in nursing homes, 6 in long-term intendance facilities and 9 in residential homes, care homes or other. Length of follow-up ranged from ane month to 11 years, with iii studies collecting information retrospectively or until death (run into Additional file 2).
Methodological quality
Fourteen of the 47 studies were judged to exist of a loftier quality, 31 of a moderate quality and 2 of a depression quality. The lowest scores on the methodological quality were on reporting the training and quality control methods for interviewers' technique (reported in 8/47 papers) and the reliability and/or validity of study instruments (reported in 8/47 papers).
Factors associated with length of stay
Factors associated with length of stay, minimum and maximum risk results and forcefulness of prove have been summarized in Table two. Three factors had strong evidence to back up their association with shorter lengths of stay: shortness of breath, receipt of oxygen therapy and access to a nursing domicile. Nine factors had moderate evidence to back up their association with shorter lengths of stay: cancer, increased contact with primary care, poor general health, poor mobility, low BMI or malnutrition, poor physical functioning, presence of pressure ulcers, older age and beingness male person.
Weak evidence to support their association with shorter lengths of stay was identified for admission from hospital, behaviour bug, biochemical indicators, poor cognitive part, dementia or Alzheimer's illness, low, diabetes, poor ambition, presence of a feeding tube, assist with feeding or nutrition, hallucinations, delusions, wandering or delirium, incontinence or catheter use, respiratory disorders or COPD, history of stroke, vision impairment, and existence married. History of fractures or falls, being of white ethnicity and vaccinations decreased the risk of shorter lengths of stay.
Subgroup analysis—studies with follow-upward periods of 1 year or less
A subgroup analysis was conducted on studies that investigated a follow-up period of one twelvemonth or less (Table 3). Twenty-six papers were included, with the same criteria as applied to the full sample. Within 1 year of follow-up, oxygen therapy remained strongly associated with shorter stays, although residence in a nursing home and shortness of breath were associated with moderate evidence. Increased age, cancer, poor appetite, being male person, poor general wellness, low BMI or malnutrition, poor physical operation remained supported past moderate evidence, respiratory disorders or COPD increased from weak to moderate evidence.
Discussion
The aim of this study was to identify factors associated with length of stay in care homes; the discussion will focus on factors identified as having strong or moderate evidence and notable exceptions.
Unsurprisingly, shorter lengths of stay were associated with characteristics related to finish of life. Shortness of breath is mutual in dying residents, and oxygen therapy provides symptom relief associated with breathlessness, both of which were supported past strong show [31]. Depression BMI and malnutrition were supported past moderate evidence, which are also common in residents approaching death [32]. Access to a facility providing nursing care was associated with shorter lengths of stay compared to a residential-only facility. It is possible that older adults admitted to residential care homes are more able to function independently than those requiring nursing care, and those who exercise crave nursing care afterwards take higher wellness needs on admission [33].
Information technology is understandable that older adults die sooner after admission; increased historic period is associated with frailty, multiple comorbidities and greater healthcare needs. Shorter lengths of stay were associated with contact with main care, which could reflect greater general practitioner involvement, either every bit resident wellness deteriorates or through the provision of palliative intendance [34]. There was inconclusive evidence to support an association between access to hospital and shorter lengths of stay. I explanation could exist that residents with a poorer diagnosis at admission may accept accelerate care planning in identify, including choosing not to be admitted to a hospital [35]. It could as well reflect variation in the services offered past different types of facilities; facilities with onsite geriatricians and nursing facilities may be better equipped to provide intendance and avoid hospital admissions compared to residential facilities; however, this cannot be explored using the current data.
There was moderate evidence to suggest that men had shorter lengths of stay in intendance homes than women. In all studies that reported the gender contour of the sample, in that location were essentially more women in the samples than men. This finding could reflect a gender imbalance in admission to intendance homes; women generally live longer than men, and the sample characteristics could reflect widowed women who are unable to live independently later on the death of a spouse [36].
Two illness diagnoses were associated with shorter lengths of stay, cancer and, at 1 year follow-up, respiratory disorders or COPD. Functional impairment and characteristics associated with poor operation, such equally poor mobility and pressure level ulcers, were identified as having moderate testify to back up them. Poor general health was associated with shorter lengths of stay, indicating that general measures of wellness and functioning may exist more accurate predictors of length of stay than individual diagnoses.
The notable finding of this review is the weak show for poor cognitive function and dementia or Alzheimer'south disease being associated with shorter lengths of stay. In Luppa et al.'southward review of predictors of care home admission, strong testify was institute to support both the association of cognitive impairment or dementia and poor concrete performance with care home access [nine], nevertheless post-admission, this review found neither cognitive impairment nor dementia nor Alzheimer's disease to be strongly associated with shorter lengths of stay.
One explanation could be related to life expectancy and illness trajectory. Compression of morbidity in ageing populations is an ongoing tendency [37], whereby the onset of chronic disease is occurring later in life, for a relatively brusk time flow before death [38]. Even so, the median survival fourth dimension for an older adult with dementia from onset to expiry is 4.i years (IQR two.five–7.half dozen) for men and 4.vi years (IQR ii.9–7.0) for women [39]. Survival varies essentially dependent on age of onset, with those diagnosed younger (between 65 and 69 years) potentially living over 10 years [39]. It is possible that residents with dementia are living longer than those with no cognitive impairment post-care abode admission.
Another explanation for these findings could exist related to characteristics prior to admission, in particular, caregiver burden. Cognitive impairment is a long-term, chronic condition, which reduces ane'due south ability to live independently. Research suggests that variation in caregiver brunt is associated with caregiver characteristics rather than patient characteristics [forty], stress among caregivers of those with dementia has been plant to exist higher than for caregivers caring for older adults without dementia [41]. Although individual experiences vary, caregivers to those with dementia provide more hours per week spent on caregiving tasks and back up a college number of activities of daily living, as well as beingness affected by negative consequences of caregiving, such as employment complications, caregiver strain and mental and physical health issues [42]. Residents with physical impairment may be surviving in the community longer than those with cognitive harm due to lower caregiver burden, and are afterwards admitted to intendance homes later, leading to shorter lengths of stay.
Finally, the availability of formal home intendance services may explain this finding. Formal home care services provide support for older adults to remain living in their own homes, undertaking domestic and personal intendance based on individual needs. It is possible that older adults with functional impairments are more than able to locate and access services to support their remaining in the customs than those with cognitive impairment, further delaying care domicile admission.
Strengths and limitations
To the authors' knowledge, this is the start systematic review of international literature on factors associated with length of stay in care homes. The review had broad inclusion criteria and was not limited to one blazon of care domicile. Efforts to ensure that the studies identified were comparable express the review to study designs that followed residents until death, meaning that residents who were discharged or moved to some other care home were not included. The inclusion of variables related to resident and care home characteristics adds an additional dimension to the review.
The review is potentially limited past the heterogeneity in the terminology used in studies in care homes. Efforts were made to include a multitude of terms related to care homes in the search strategy used to identify studies from a multifariousness of settings; withal, it is possible that some studies that included less common terms for care homes were missed. The levels of care provided by different care homes, their admission criteria and the terminology used to define care homes vary between countries making the synthesis of information published on intendance homes problematic. For case, the definition of long-term intendance facilities applied in this review excluded studies in assisted living facilities and sheltered adaptation. Farther give-and-take is needed to refine the terms used in this surface area and meliorate subsequent reporting. In addition, it is difficult to make meaningful comparisons between countries without considering the national policies and provision of care offered by intendance homes inside a country's wider wellness intendance system. The review besides does non capture a resident's living arrangement prior to admission that may affect the decision to enter a care dwelling house and their subsequent experience.
The focus of the review centered on studies that had explored a number of factors as their aim, without whatever prior hypothesis. Studies that explored the part of one cistron on length of stay, such as low or malnutrition, were excluded, for ii reasons. Firstly, it would be incommunicable to develop a search strategy that could identify all factors associated with length of stay, without first having a basis on which to justify the inclusion of search terms for each gene. Secondly, the number of studies identified would be very large and difficult to synthesize.
The interpretation of the results is also limited by the limitations of the individual studies. Most studies only collected data at baseline, with follow-upwardly restricted to the outcome measure of time until decease. It is possible that changes in time-dependent characteristics, such as cognitive damage, which may get progressively worse, were missed. There were numerous measures used to assess factors, for example, at least vi tools were used to assess physical functioning and 12 for cerebral functioning; all the same, the analytical approach used in this review allowed these findings to exist combined and weighted into a meaningful measure of association and methodological quality. Finally, the review did non perform report selection and study extraction in duplicate on the full dataset.
Implications for further research
The written report highlighted the varied trajectories of care domicile residents approaching end of life and the need for flexible, appropriate palliative care provision to accommodate unlike trajectories. This review has synthesized factors associated with variation in length of stay in care homes, and identified like homogeneity within the care dwelling population from access to expiry, which is not yet fully understood.
Increasingly, care homes are taking on a complex role within the wider health organization, catering for the diversities of an ageing population that can no longer live in the community. At 1 end of the spectrum, care homes are acting every bit proxy hospices for brusk-stay residents budgeted terminate of life. At the other end, care homes are accommodating residents with cognitive impairments who may survive for many years mail service-access. Supporting care homes in negotiating these two roles; delivering palliative care for brusk-stay residents while simultaneously providing a residential home for long-stay residents, in the same space, is imperative and requires further research. In add-on, farther idea should be given to the suitability of care homes in catering for such a broad variation in needs. The potential for other types of services, such equally specialist dementia care units and assisted living facilities, in providing care for subgroups of care dwelling house residents could be examined, although there is argue as to whether such services provide better intendance [43, 44].
The findings of this review accept identified numerous questions requiring further investigation. Firstly, further inquiry is needed to explore the relationship between factors associated with care home admission and factors associated with length of stay. Longitudinal studies which follow community-home older adults mail service-access are required to fully sympathise this relationship. Secondly, in this review, characteristics related to the care home were simply nerveless in viii studies, further data on variation in length of stay and care abode-related factors could identify means to improve the commitment of care. It is imperative that research on intendance home residents contextualizes the data within the long-term intendance setting to inform the generalizability of the findings internationally. Finally, inclusion and identification of intendance home residents in existing national datasets would allow comparisons within and between countries, and enable time-dependent variables to be monitored.
Conclusion
Care home residents remain a growing, diverse population. An agreement of the factors associated with shorter and longer lengths of residence within intendance homes tin can exist used to inform residents and their families most their potential use of health intendance services. Clinicians can use these findings to inform treatment decisions for older residents residing in intendance homes, and if required, organize palliative care. On a wider scale, policy-makers tin can use these findings to inform service planning for the time to come and to identify facilities in which lengths of stay deviate from the expected. Skilful quality, replicable research on the wellness needs of care home residents is a priority, at present and in the future.
Abbreviations
- BMI:
-
Torso mass index
- COPD:
-
Chronic obstructive pulmonary disease
References
-
Un Department of Economic and Social Affairs Population Division. World Population Ageing 2017 - Highlights. 2017. New York: ST/ESA/SER.A/397.
-
United Nations Department of Economical and Social Affairs Population Sectionalisation. World Population Prospects: the 2017 Revision.2017.New York: ESA/P/WP/248 2017.
-
Mathers CD, Loncar D. Projections of global bloodshed and burden of disease from 2002 to 2030. PLOS Med. 2006;3(11):e442.
-
Gomes B, Calanzani Northward, Gysels Thou, Hall S, Higginson I. Heterogeneity and changes in preferences for dying at abode: a systematic review. BMC Palliat Care. 2013;12:vii.
-
Houttekier D, Cohen J, Bilsen J, Addington-Hall J, Onwuteaka-Philipsen BD, Deliens L. Place of death of older persons with dementia. A study in five European countries. J Am Geriatr Soc. 2010;58(4):751–6.
-
Mitchell SL, Teno JM, Miller SC, Mor 5. A National Written report of the location of decease for older persons with dementia. J Am Geriatr Soc. 2005;53(2):299–305.
-
Os AE, Gomes B, Etkind SN, Verne J, Murtagh FEM, Evans CJ, et al. What is the impact of population ageing on the future provision of end-of-life care? Population-based projections of place of death. Palliat Med. 2018;32(2):329–36.
-
Froggatt K, Reitinger E. Palliative intendance in term care settings for older people. Study of an EAPC taskforce 2010–2012. European Association of Palliative Care: Milan; 2013.
-
Luppa G, Luck T, Weyerer Southward, König H-H, Brähler E, Riedel-Heller South. Prediction of institutionalization in the elderly. A systematic review. Age Ageing. 2010;39(1):31–8.
-
Shah SM. Identifying the clinical characteristics of older people living in care homes using a novel approach in a master care database. Age Ageing. 2010;39:617–23.
-
Groom 50, Avery AJ, Boot D, O'Neill C, Thornhill One thousand, Brown Chiliad, et al. The bear upon of nursing home patients on general practitioners' workload. Br J Gen Pract. 2000;50(455):473–6.
-
Godden South, Pollock AM. The use of acute hospital services past elderly residents of nursing and residential care homes. Health Soc Intendance Community. 2001;nine(six):367–74.
-
Graverholt B, Forsetlund Fifty, Jamtvedt Grand. Reducing infirmary admissions from nursing homes: a systematic review. BMC Wellness Serv Res. 2014;14:36.
-
Barclay S, Froggatt K, Crang C, Mathie E, Handley K, Iliffe S, et al. Living in uncertain times: trajectories to death in residential intendance homes. Br J Gen Pract. 2014;64(626):e576–e83.
-
Enquiry Data Assistance Center. Long Term Care Minimum Data Ready 3.0. Minneapolis, USA: Research Information Assistance Heart; 2018 [Available from: http://www.resdac.org/cms-data/files/mds-3.0. Accessed 1 Sept 2018.
-
The Found for Fiscal Studies. English longitudinal written report of ageing. London, United kingdom: Institute for Fiscal Studies; 2018 [xi/01/2018]. Available from: http://www.ifs.org.united kingdom/ELSA. Accessed one Sept 2018.
-
Boersch-Supan A, Brandt Thousand, Hunkler C, Kneip T, Korbmacher J, Malter F, et al. Data resource profile: the survey of wellness, ageing and retirement in Europe (SHARE). Int J Epidemiol. 2013;42(4):992–1001.
-
Collingridge Moore D, Hanratty B. Out of sight, out of mind? A review of information bachelor on the health of care domicile residents in longitudinal and nationally representative cross-sectional studies in the UK and Ireland. Age Ageing. 2013;42(6):798–803.
-
Hall S, Longhurst S, Higginson IJ. Challenges to conducting research with older people living in nursing homes. BMC Geriatr. 2009;nine:38.
-
Reitinger E, Froggatt K, Brazil Grand, Heimerl K, Hockley J, Kunz R, et al. Palliative care in long-term intendance settings for older people : findings from an EAPC taskforce. Eur J Palliat Care. 2013;20(5):251–3.
-
Froggatt K, Edwards M, Morbey H, Payne Due south. Mapping palliative care systems in long term intendance facilties in Europe Lancaster. Britain: Lancaster University; 2016.
-
Kruse RL, Oliver DP, Mehr DR, Petroski GF, Swenson DL, Zweig SC. Using mortality hazard scores for long-term prognosis of nursing domicile residents: caution is recommended. J Gerontol Ser A Biol Sci Med Sci. 2010;65A(11):1235–41.
-
Porock D, Parker-Oliver D, Petroski GF, Rantz M. The MDS mortality adventure index: the development of a method for predicting 6-month bloodshed in nursing domicile residents. BMC Res Notes. 2010;iii:200.
-
Mitchell Due south, Miller S, Teno J, Kiely D, Davis R, Shaffer Thousand. Prediction of half dozen-month survival of nursing habitation residents with advanced dementia using ADEPT vs hospice eligibility guidelines. JAMA. 2010;304(17):1929–35.
-
Thomas JM, Cooney LM, Fried TR. Systematic review: health-related characteristics of elderly hospitalized adults and nursing home residents associated with curt-term mortality. J Am Geriatr Soc. 2013;61(vi):902–eleven.
-
Moher D, Liberati A, Tetzlaff J, Altman D for the PRISMA group. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA argument. BMJ. 2009;339:b2535.
-
Vandenbroucke JP, von Elm E, Altman DG, Gotzsche PC, Mulrow CD, Pocock SJ, et al. Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) explanation and elaboration. Epidemiology. 2007;eighteen(6):805–35.
-
Engle VF, Graney MJ. Predicting outcomes of nursing-home residents - death and discharge home. J Gerontol. 1993;48(5):S269–S75.
-
Hedinger D, Hammig O, Bopp G, Swiss National Cohort Study G. Social determinants of duration of final nursing abode stay at the cease of life in Switzerland: a retrospective cohort study. BMC Geriatr. 2015;xv:114.
-
Sanderson South, Tatt LD, Higgins JPT. Tools for assessing quality and susceptibility to bias in observational studies in epidemiology: a systematic review and annotated bibliography. Int J Epidemiol. 2007;36(3):666–76.
-
Qaseem A, Snowfall Five, Shekelle P, Casey DE, Cantankerous JT, Owens DK, et al. Evidence-based interventions to improve the palliative care of pain, dyspnea, and low at the end of life: a clinical practice guideline from the American College of Physicians. Ann Intern Med. 2008;148(2):141–6.
-
Suominen M, Muurinen Southward, Routasalo P, Soini H, Suur-Uski I, Peiponen A, et al. Malnutrition and associated factors amid anile residents in all nursing homes in Helsinki. Eur J Clin Nutr. 2005;59(four):578–83.
-
Darton R, Bäumker T, Callaghan Fifty, Holder J, Netten A, Towers A-Thou. The characteristics of residents in actress care housing and intendance homes in England. Health Soc Care Customs. 2012;twenty(1):87–96.
-
Mitchell Due south, Loew J, Millington-Sanders C, Dale J. Providing end-of-life intendance in full general practice: findings of a national GP questionnaire survey. Br J Gen Pract. 2016;66(650):e647–e53.
-
Caplan GA, Meller A, Squires B, Chan S, Willett W. Accelerate care planning and hospital in the nursing dwelling. Age Ageing. 2006;35(half dozen):581–five.
-
Glaser K, Grundy East, Lynch K. Transitions to supported environments in England and Wales among elderly widowed and divorced women: the changing balance between co-residence with family and institutional care. J Women Aging. 2003;15(2–iii):107–26.
-
Chatterji South, Byles J, Cutler D. Health, functioning, and disability in older adults-present status and time to come implications. Lancet. 2015;385(9967):508.
-
Chips JF. Measuring and monitoring success in compressing morbidity. Ann Intern Med. 2003;139(5):455–9.
-
Xie J, Brayne C, Matthews FE. Medical Inquiry Council. Survival times in people with dementia: analysis from population based cohort study with 14 year follow-upward. Br Med J. 2008;336(7638):258–62.
-
Garlo K, O'Leary JR, Van Ness PH, Fried TR. Burden in caregivers of older adults with advanced illness. J Am Geriatr Soc. 2010;58(12):2315–22.
-
Bertrand RM, Fredman Fifty, Saczynski J. Are all caregivers created equal? Stress in caregivers to adults with and without dementia. J Crumbling Wellness. 2006;18(iv):534–51.
-
Ory MG, Hoffman RR, Yee JL, Tennstedt S, Schulz R. Prevalence and bear upon of caregiving: a detailed comparing between dementia and nondementia caregivers. Gerontologist. 1999;39(2):177–85.
-
Reilly S, Abendstern One thousand, Hughes J, Challis D, Venables DAN, Pedersen I. Quality in long-term care homes for people with dementia: an assessment of specialist provision. Ageing Soc. 2006;26(4):649–68.
-
Sloane PD, Zimmerman Southward, Gruber-Baldini AL, Hebel JR, Magaziner J, Konrad TR. Wellness and functional outcomes and wellness care utilization of persons with dementia in residential intendance and assisted living facilities: comparing with nursing homes. Gerontologist. 2005;45(one):124–34.
Acknowledgements
We are grateful to the authors who responded to our requests for further data about their inquiry.
Funding
The atomic number 82 author received funding from the Eu's 7th Framework Programme (FP7/ 2007-2013) under grant agreement 603111 (Pace project Palliative Intendance for Older People). The funders had no office in study design, drove, analysis or estimation of the information, nor in writing and the decision to submit this commodity for publication.
Availability of data and materials
The search strategies used during the electric current study are available from the respective author on reasonable request.
Author information
Affiliations
Contributions
DCM designed the protocol, conducted the search, reviewed the papers for inclusion, extracted and synthesized the information and wrote the paper. LD acted as a second reviewer. Supervising authors interpreted data and critically reviewed the paper. All authors read and canonical the final manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
Non applicable.
Consent for publication
Not applicative.
Competing interests
The authors declare that they take no competing interests.
Publisher'south Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Boosted files
Additional file 1:
Criteria for assessing methodological quality of studies. (DOCX 34 kb)
Additional file ii:
Factors associated with length of stay before expiry in intendance home residents in all studies and separate between high-, moderate- and low-quality studies. (DOCX 45 kb)
Additional file 3:
Factors associated with length of stay before death in intendance home residents in all studies and split up between high-, moderate- and low-quality studies-limited to 1 year follow-upwards. (DOCX 47 kb)
Additional file 4:
Factors associated with length of stay before death in care abode residents—data extracted from included papers. (DOCX 349 kb)
Rights and permissions
Open up Access This article is distributed under the terms of the Creative Eatables Attribution four.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in whatever medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and signal if changes were fabricated. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/i.0/) applies to the information made available in this article, unless otherwise stated.
Reprints and Permissions
About this commodity
Cite this commodity
Moore, D.C., Keegan, T.J., Dunleavy, Fifty. et al. Factors associated with length of stay in intendance homes: a systematic review of international literature. Syst Rev viii, 56 (2019). https://doi.org/10.1186/s13643-019-0973-0
-
Received:
-
Accepted:
-
Published:
-
DOI : https://doi.org/10.1186/s13643-019-0973-0
Keywords
- Systematic review
- Long-term care facility
- Care abode
- Nursing dwelling
- Length of stay
Source: https://systematicreviewsjournal.biomedcentral.com/articles/10.1186/s13643-019-0973-0
0 Response to "Covid-19 Length of Hospital Stay a Systematic Review and Data Synthesis"
แสดงความคิดเห็น